Quick Start
- Go to Eligibility Checks in the left menu.
- Click New Eligibility Check.
- Enter the patient’s First Name, Last Name, Date of Birth, and Member ID.
- Enter your Provider NPI.
- Select the Insurance Payer.
- Set the Date of Service and Service Type.
- Click Verify Insurance.
Step-by-Step
Opening a New Check
-
Go to the left menu and click Eligibility Checks.
-
Click the New Eligibility Check button in the top right corner.
Entering Patient Information
If the patient already exists in Solum, use the Search existing patient bar at the top to find and pre-fill their details. If the patient has not been created in Solum yet, enter their information manually:- Fill in the following fields:
| Field | Required | Description |
|---|---|---|
| First Name | Yes | Patient’s first name as it appears on their insurance card |
| Last Name | Yes | Patient’s last name as it appears on their insurance card |
| Date of Birth | Yes | Patient’s date of birth in MM/DD/YYYY format |
| Member ID | Yes | The member ID from the patient’s insurance card |
Provider and Insurance Information
- Enter your Provider NPI in the Provider Information section:
Your NPI is a 10-digit number. If you’re unsure which NPI to use, check with your billing team or contact support@getsolum.com.
- Select the Insurance Payer from the dropdown.
Encounter Information
- Select the Date of Service.
- Select the Service Type from the dropdown.
For general health benefits, you can use Service Type 30. We recommend running only one service type at a time for the most accurate results.
Examples:
ABA: CF
Speech Therapy: AF
Occupational Therapy: AD
Physical Therapy: PT
Examples:
ABA: CF
Speech Therapy: AF
Occupational Therapy: AD
Physical Therapy: PT
Running the Check
- Click the Verify Insurance button.
Reviewing Results
-
Once the check is completed, you will see the eligibility results on screen. At the top, you will see whether the patient’s coverage is Active or Inactive.



Overview Tab
The Overview tab gives you a high-level summary of the eligibility response. It is organized into the following sections:| Section | What It Shows |
|---|---|
| Subscriber | Patient’s name, date of birth, gender, Member ID, group number, and address |
| Encounter | The service type codes and date of service used in the check |
| Provider | The organization name and NPI used for the verification |
| Payer | The insurance company name and payer ID |
| Plan | Plan name, insurance type (e.g., PPO, HMO), group number, group description, and plan begin/end dates |
| Benefit - Related Entities | Organizations involved in managing the patient’s benefits, including contact numbers and associated benefit types |
The Benefit - Related Entities section can show important details like Utilization Management Organizations. For example, if physical therapy benefits are managed by a separate organization, their contact number will appear here. This is useful when you need to call for prior authorization or additional benefit details.
Benefits Tab
The Benefits tab shows the full detail of the patient’s coverage. This is where you find deductibles, copays, coinsurance, and any limitations. The benefits are displayed in a table. You can filter the results using the filter buttons at the top of the page: Type Filter — Filter benefits by category:| Type | What It Means |
|---|---|
| Statuses | Whether the coverage is active or inactive |
| Co-Insurance | The percentage the patient pays after meeting their deductible |
| Co-Payment | A fixed dollar amount the patient pays per visit |
| Deductible | The amount the patient must pay before insurance begins covering services |
| Limitations | Visit limits, dollar caps, or other restrictions on coverage |
| Non-Covered | Services or procedures not covered under the patient’s plan |
| Out of Pocket (Stop Loss) | The maximum amount the patient will pay in a year before insurance covers 100% |
| Benefit Disclaimer | Important notices from the payer about the benefits response |
- Employee Only — Benefits for the subscriber only
- Individual — Benefits for one covered person
- In-network — Benefits when the provider is in the payer’s network
- Out-of-network — Benefits when the provider is out of network
- Both — Benefits that apply regardless of network status
- Not set — The payer did not specify a network indicator
Matching Results to a Patient
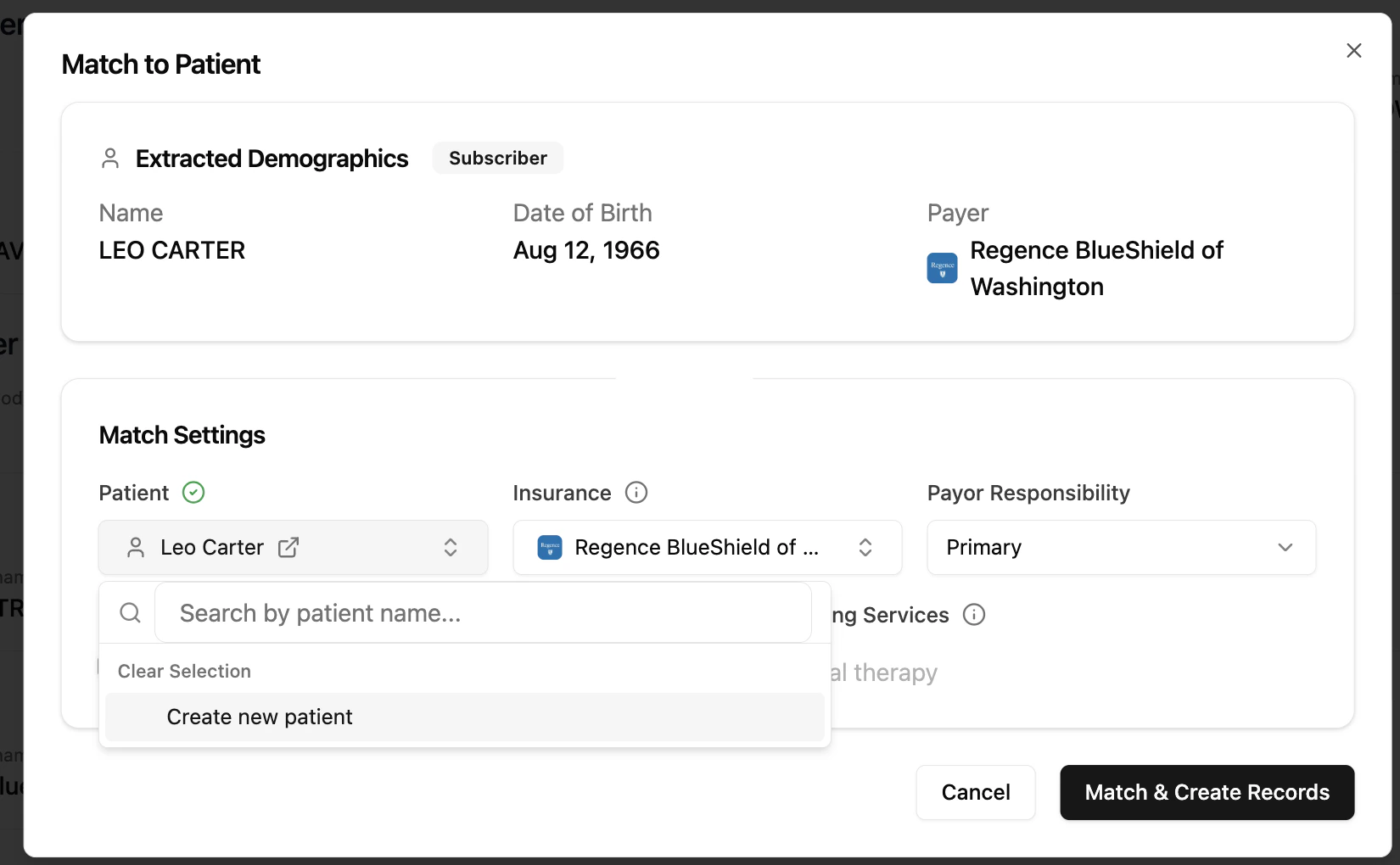
- Click Match to Patient at the top of the results page.
- Review the insurance information. You can adjust it if needed, or click Create New Insurance Automatically to use the details returned by the payer.
- Confirm the Payor Responsibility (Primary, Secondary, or Tertiary).
-
Click Match & Create Records.
After Matching
- Go to the Workflow section in the left menu.
- Click on the patient profile to view their details.
Troubleshooting
| Problem | Fix |
|---|---|
| Check returns a Failed status | Double-check that all patient info matches exactly what’s on the insurance card. Remove any middle names from the First Name field. |
| Payer not found in the dropdown | Email support@getsolum.com with the payer name and the Solum team will help identify the correct option. |
| Results show inactive coverage | Verify the Member ID and Date of Birth are correct. The patient’s coverage may have lapsed or changed. |
| Unsure which NPI to use | Select from the dropdown if your locations are configured, or see Adding Locations & Credentialing. |
| Results are incomplete or missing benefit details | Some payers only return basic coverage confirmation. For full benefit details, a manual Verification of Benefits (VOB) call may be needed. |
| Benefits table is hard to read | Use the Type, Network, and Service or Procedure filters at the top to narrow the results. Click Match to Patient to see a cleaner view organized by service type. |

